
Intelligent homes: empowering people to “live well” with dementia

The UK Dementia Research Institute is a first-of-its-kind national initiative focused on science and discovery to address the main forms of neuro-degeneration – with the ambition of improving diagnosis, treatment, well-being and, ultimately, enabling prevention of these debilitating conditions. We spoke with Imperial College London’s Professor Tim Constandinou – UK DRI Group Leader within the UK DRI Care Research & Technology Centre based in White City Innovation District – about his work developing breakthrough bioelectronic systems for intervention in dementia, and the role of technology innovation in empowering people with dementia to live safely, healthily and independently.
The UK Dementia Research Institute (UK DRI) is marking the first five years of its mission to uncover new knowledge and unlock urgent treatments for all dementias, including Alzheimer’s disease, Parkinson’s disease, vascular dementia, Lewy body dementia, Parkinson’s dementia, motor neurone disease, Amyotrophic Lateral Sclerosis (ALS) and beyond. Dementia currently affects more than 45 million people worldwide, with a new case diagnosed every three seconds.
Launched in 2017, the UK DRI is the single biggest investment the UK has ever made in dementia, thanks to founding funders the Medical Research Council (MRC), Alzheimer’s Society and Alzheimer’s Research UK.
The Institute is bringing together world-leading expertise in neuroscience, biomedical, care and translational dementia research into a national institute that is uniquely structured across seven UK centres, with its more than 750 researchers able to share scientific inspiration and coordinate partnerships.
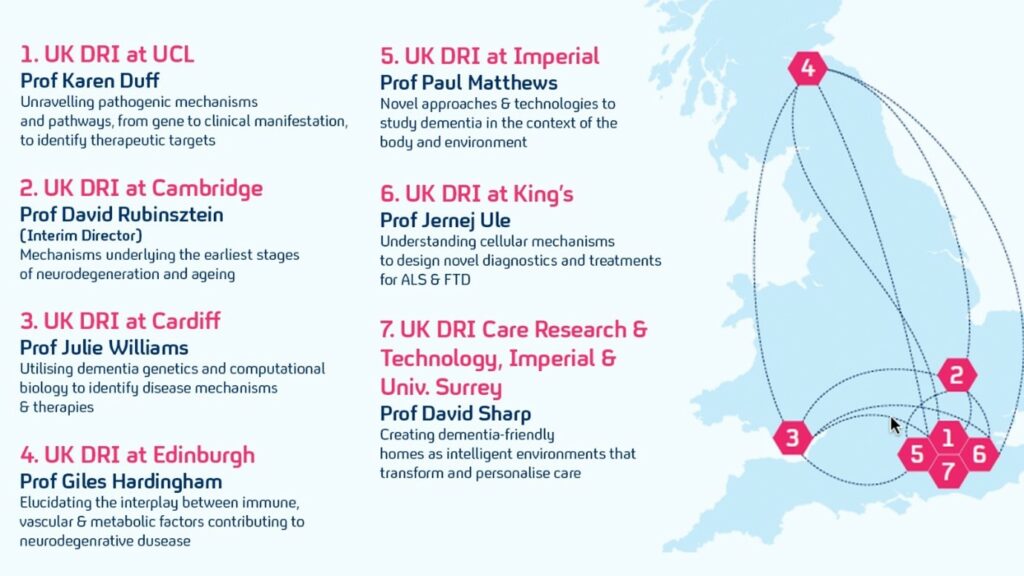
One of two major centres based at Imperial College London is UK DRI Care Research & Technology, led by Professor David Sharp in partnership with University of Surrey. This state-of-the-art, multi-disciplinary research centre, located at The Sir Michael Uren Hub in White City Campus, draws together a diverse team of doctors, engineers and scientists to harness recent advances in artificial intelligence, engineering, robotics and sleep science, with the aim of creating new technologies that will deliver the highest quality dementia care in the home. Together, this world-class team of researchers are investigating new ways to keep people independently in their homes, improve their general health and sleep, and reduce the distress, confusion and agitation that can often attend dementia-related conditions.
Timothy Constandinou – Professor of Bioelectronics at Imperial College London, Director of the Next Generation Neural Interfaces (NGNI) Lab, and Head of the Circuits & Systems (CAS) Research Group at Imperial College London – is Group Leader at the UK DRI Care Research & Technology Centre based at Imperial, where he leads an exciting programme that is developing unobtrusive radar sensors, in-ear hearables, plus implantable devices to empower next-generation dementia care and research.
Q: Tim, how would you describe the overall mission of your research group?
A: Within our group, we’re looking at how to improve care for people with dementia, and also how to make the lives of their carers easier, through developing new devices that we can put directly into people’s homes for 24/7 monitoring and intervention.
Our work is focused on the creation of novel bioelectronic systems that will enable continuous, minimally obtrusive monitoring and interventions that can improve outcomes for people with dementia, and we’re also looking at how we can facilitate and impact clinical research. A key part of that is exploring how we gather data from people with dementia – information that isn’t currently available – in an effective way.
Q: Can you talk us through some of your current projects?
A: Right now, our centre is trialling an innovative smart home system called Minder. Professor David Sharp, our Centre Director, is a neurologist and is driving a highly translational and clinically-led approach to the development programme.
The Minder kit is intended for deployment in people’s home to provide continuous monitoring that can not only enable interventions, but also improve the quality of data that medical professionals have to work on, and also inform research studies. We are working on the core infrastructure of this system in partnership with a service provider.
An illustrative use of the Minder system could be to predict and detect urinary tract infections (UTIs) before they become too severe, just by looking at how many times a person is going to the bathroom and analysing patterns of movements around the home. Picking up the probability of UTIs early allows medical professionals to deploy a proper test, prescribe antibiotics immediately, and prevents people from having to be admitted into hospital, which is expensive for health service providers and, for dementia patients themselves, can sometimes mean coming out in a worse condition than when they went in.
Another key challenge that the Minder system is seeking to address spans elderly care in general, which is that patients are sometimes not able to give caregivers or medical professionals a reliable history of what has happened, or of their state. An app that can tell you whether the person is turning on their kettle every morning, or regularly taking their medication, provides both peace of mind and a level of early detection that would be extremely valuable both in the home and in institutional or care home settings.
The Minder infrastructure we’re deploying could be used for detecting and predicting falls through activity sensors, and providing context and history as to how the fall actually happened. Gathering these streams of data together in real-time could allow us to pick up and flag potential patterns, and even prevent falls by triggering an emergency SOS and alerting a monitoring team.
For medical professionals, this system could provide a high level of data that could be used to annotate patient records, for example, delivering vital information for the assessment of interventions, the efficacy of new medicines and whether they are succeeding in slowing down neuro-degeneration, whether Parkinson’s drugs are proving effective in movement, and so on. This allows the possibility of altering the environmental conditions and adjusting things in such a way that quality of care can be improved based on real data.
Q: What stage is your research, and what are the big research challenges ahead?
A: We currently have the Minder infrastructure deployed live in 70 real homes. We’re currently using off-the-shelf sensors on doorways to sense, for example, when the kitchen door opens, and some of our sensors are functioning as smart plugs. We’re harnessing passive infra-red sensors to monitor human motion, and we’re using once-a-day medical sensors – blood pressure sensors, pulse oximetry and so on – to provide a rich dataset from multiple sources. This data is then sent to our cloud infrastructure and Machine Learning and Artificial Intelligence is applied over long periods of time to enable the detection of patterns, for example, sleep quality and how pharmacological interventions are affecting behaviour.
What we would we like to do is to be able to monitor more physiological parameters – blood pressure, heart rate, breathing and behavioural parameters, for example, plus precise movement patterns, whether the person is watching TV, if they are sleeping in bed or on the sofa and so on. We’d also like to monitor posture in an unobtrusive way, to assess whether the individual’s level of frailty and mobility. To do this effectively, it would have to be completely unobtrusive, and not burden the person with dementia or their carers. Moreover, it would need to be deployable in a way that respects privacy – so, without cameras.
One of the technologies we are exploring for this is a low-cost radar technology in every room that can sense the motion of objects around a person in an omni-directional fashion. The challenge is to make this radar technology low-cost in terms of sensors, and comparable with passive infra-red. It could be used to sense certain parameters – looking at a person’s position in a room, the speed of their gait, how they are walking down a corridor – and identify patterns and monitor changes in trends. This could prove extremely useful for areas such as gait cycle assessment and assessing levels of frailty in an automated manner. Similarly, it would have great utility in sleep physiology and examining quality of sleep.
Our goal for the next few years is to continue working with our cohort of patients to improve the quality of data, deploy the technology more widely, and to begin talking with local councils to see how innovation this can be scaled up – from an ecosystem perspective, from a funding perspective, from a device manufacturing perspective, and in terms of the best ways for doctors and health professionals to access the data. It’s at a very exciting phase.
Q: How does being based in White City Innovation District benefit your research?
A: By being located within WCID, we’re in the same building as the bioengineering department, and we also share a floor with the British Heart Foundation Centre of Research Excellence, so there are a lot of important synergies. Directly next door to us is the I-HUB and the London Biofoundry, which links closely to our biosensor development, so that co-location is really valuable for pushing our programmes forward.
We’ve also been able to create a multi-disciplinary “Living Lab” in White City Campus – an apartment that is fitted out with the sensors that we typically deploy in people’s homes. The entire floor of the apartment is pressure-sensitive, so we can monitor where and how people are standing, and we have depth cameras that can look at people’s limb movements to develop wireframe images for further study. With this lab, which is focused primarily on activities and daily living, we can accurately assess new technologies compared to “ground truths”. The DRI facility at Surrey has a similar lab that is focused on sleep science. Our current trials are studying a group of elderly participants, some of which may have chronic conditions – but not dementia – and the next cohort intake is likely to be people with early-stage dementia or mild cognitive impairment.
We’re also working in partnership with the Helix Centre at St Mary’s Hospital, talking widely with carers, patients and clinicians to make sure that our ideas and technologies are fit for purpose. As many user requirements and preferences are taken into account at the very early stages of development, so that we can ensure whatever we innovate delivers real value and improves people’s lives in the real world.
“By developing new devices enabling passive and minimally obtrusive sensing, as well as bioelectronic intervention, we aim to deploy technology that provides new insights to ultimately improve the lives of people living with dementia.”
Professor Timothy Constandinou, UK DRI Group Leader
To discover more about the mission and work of the UK Dementia Research Institute, visit:
UK DRI: UK Dementia Research… | UK DRI: UK Dementia Research Institute
For the UK DRI Centre at Imperial College London, head to: UK DRI Centre at Imperial | Research groups | Imperial College London
Explore the current research from UK DRI Care Research & Technology: Care Research & Technology | UK DRI: UK Dementia Research Institute
